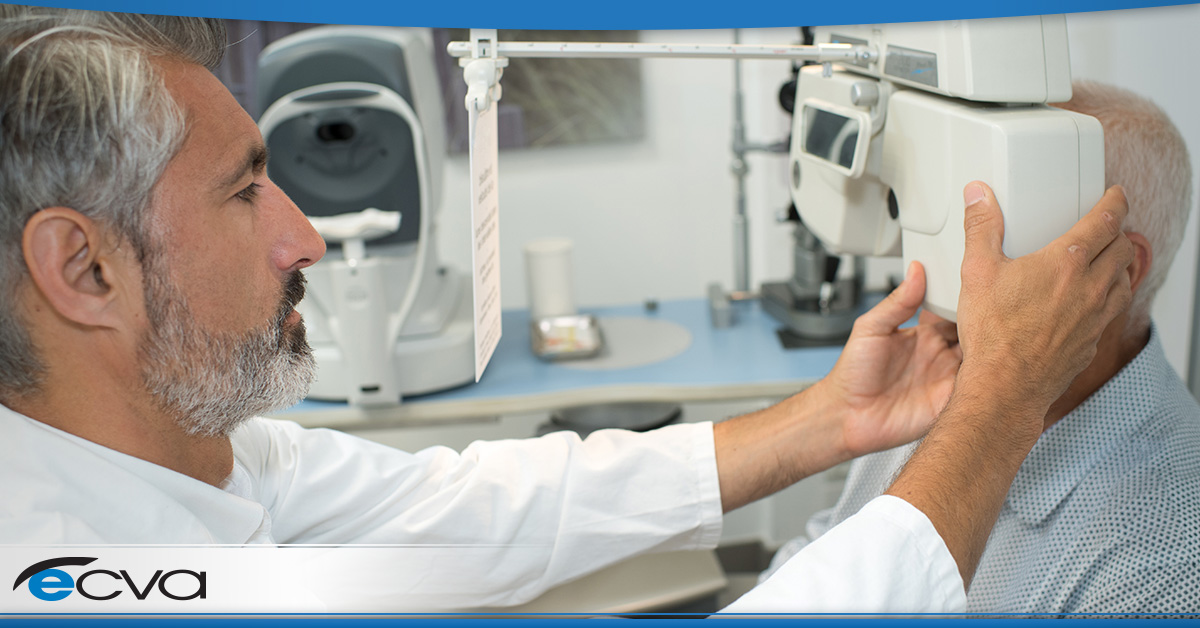
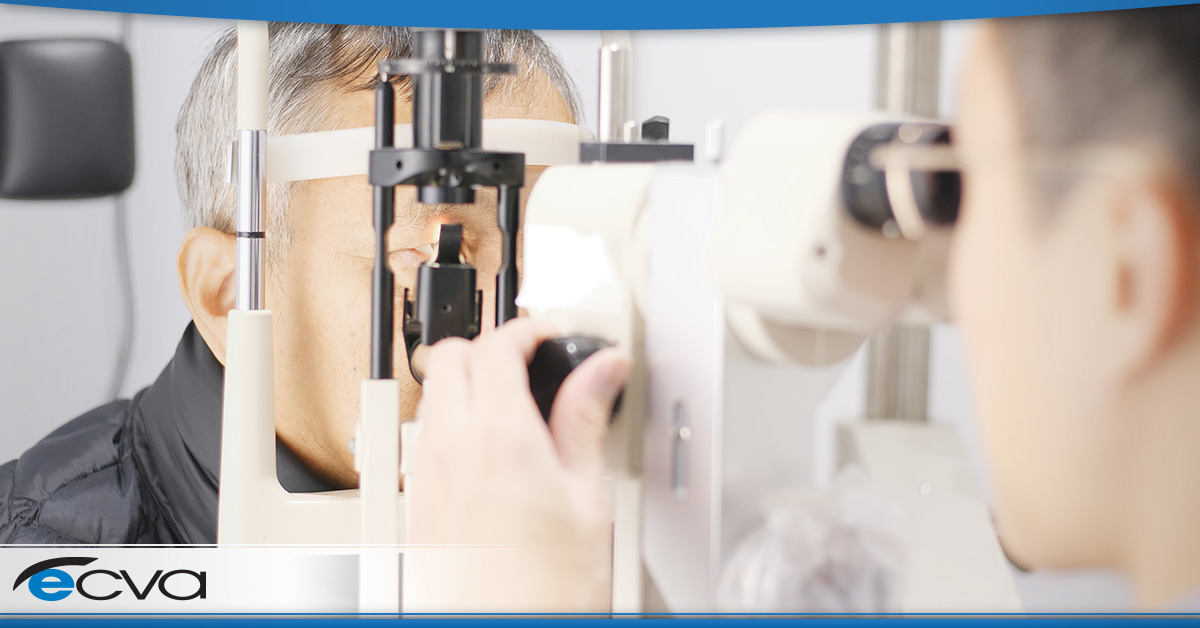
Cataract surgery is among the most common types of surgery. While it was once an inpatient procedure requiring general anesthesia, it can now be performed under local anesthesia on an outpatient basis. This approach is more convenient, safer, and less expensive, and cataract surgery success rates have never been higher. Traditionally, cataract surgery has been performed with a scalpel, but lasers are increasingly used. Patients report little pain and a quick recovery in most cases. Cataract surgery success rates are very high, reportedly 97-98%, according to recent studies, and few complications are encountered.
Who Performs Cataract Surgery?
If you’re looking for an eye doctor for cataracts, ophthalmologists are the specialists who perform this type of surgery. If you’ve never had eye surgery before, your eye care has most likely been managed by optometrists or opticians. Optometrists are licensed professionals who can perform eye examinations and diagnose and treat some conditions, but they are not medical doctors. Conditions that require surgery, such as cataracts, must be referred to an ophthalmologist. If you have glasses or contacts, you’ll know your optician as the helpful person who ensures they fit correctly.
What are the Risks of Cataract Surgery?
Any surgery comes with a degree of risk, but cataract surgery complications are rare and seldom serious. All long as the patient follows the post-operative instructions their ophthalmologist gives them, the chances they will experience any side effects are low. There are three serious potential issues to be aware of: retinal detachment, swelling of the eye and eye infection. Familiarize yourself with the following symptoms and report any occurrences to your ophthalmologist immediately. While these cataract surgery complications are serious if ignored, prompt treatment can keep you and your vision healthy.
Retinal Detachment
Cataract surgery has been shown to cause a slightly increased risk of retinal detachment. For patients with other eye disorders, such as high myopia – a rare type of severe nearsightedness – the risk of retinal detachment is even higher. Left untreated, it can lead to permanent vision loss.
Retinal detachment is usually painless. The symptoms you are likely to notice are a sudden increase in floaters or flashes of light. Floaters are just what they sound like – little specks that seem to float around in your vision. If you notice these symptoms, don’t take a nap or wait to see if they clear up on their own, contact your doctor immediately, even if they occur after hours. The sooner retinal detachment is treated, the better the chances of preserving some or all of your vision.
Swelling of the Eye
Some post-surgical swelling of the eye is not unusual. It can increase during the first 24 hours after surgery. It can be alarming to notice that your vision was better immediately right after surgery than a day later. Chances are, the swelling will go down on its own, but if it’s severe and not dissipating as your instructions indicated that it would, don’t hesitate to contact the ophthalmologist who performed your cataract surgery. They may tell you to use your steroid eye drops more frequently or prescribe something different or more potent.
Eye Infection
Preventing eye infection often comes down to meticulous hygiene. Your ophthalmologist will do their part by prescribing antibiotic drops for you to begin using before surgery and continue afterward. You can do your part by using the drops as prescribed and washing your hands well with soap before using the drops or touching the eye area. Also, take care not to touch the surface of your eye or your eyelashes with the dropper.
Is Cataract Surgery Always Successful?
While the cataract surgery success rate is high, it’s not 100%. It’s possible for your vision to be worse than before the surgery or blurry. Typically, this is due to issues such as waiting too long to have cataract surgery performed, which can lead to difficulties with the surgery.
Can Cataracts Come Back After Surgery?
Once cataracts are removed, they cannot grow back, but a new one can form. These secondary cataracts are called posterior capsular opacification(PCO). Secondary cataract symptoms take months or years to develop and are becoming rarer as technology has advanced. Reasons for an increased risk of PCO include age (secondary cataract symptoms are more common among younger patients), diabetes, uveitis, myotonic dystrophy, and retinitis pigmentosa. Cataracts caused by injury are more likely to lead to secondary contact symptoms.
Secondary cataract symptoms to watch for include blurry vision, glare or halos from headlights and issues with vision such as trouble reading, driving, watching television and sometimes difficulty with color perception. If you notice any of these symptoms, contact your cataract ophthalmologist.
How Long Does it Take to Recover From Cataract Surgery?
After cataract surgery, most people can go back to work and resume other daily activities in a couple of days. Full recovery can take as long as eight weeks and your vision should stabilize within 3-6 weeks. The closer you follow the instructions of your ophthalmologist, the better your chance of being a cataract surgery success story.
What Should You Look For in a Cataract Surgeon in Buffalo?
When you’re trusting someone with your vision, you want an ophthalmologist you can trust. Look for a surgeon specializing in cataract surgery and up to date on the latest studies and technologies. Look for reviews and recommendations and review the credentials and experience of any cataract surgeon you consider. Be sure to ask your surgeon relevant questions such as how many surgeries they have performed and their cataract surgery success rate.
Credentials of a Cataract Surgeon
Your surgeon should be board certified in ophthalmology if they have the training and skills required to perform cataract surgery successfully. You should also check that the doctor has no malpractice suits or disciplinary actions on their record. Healthgrades.com is a good source for conducting this research.
Experience
Even though cataract surgery is relatively simple and risk-free, you don’t want to put your eyesight in the hands of someone who doesn’t have plenty of experience. Surgery performed by an ophthalmologist with plenty of experience increases the chances of successful cataract surgery. A doctor who has performed the surgery many times before will know exactly what to watch for.
Choosing the Right Cataract Surgeon in Buffalo
If you have been identified as a candidate for cataract surgery, you may wonder what the next step is. If an optometrist diagnosed you, they may refer you to a specific ophthalmologist, or provide you with a list to choose from. If they did not refer you, there are several ways to find qualified cataract ophthalmologists in Buffalo. If you have friends or family who have undergone cataract surgery, they may be able to provide recommendations for cataract eye doctors in Buffalo. If not, your insurance company may be able to help, or you can request referrals from the American Academy of Ophthalmology.
At ECVA, the safety and health of our patient’s eyes and vision are our priority. That’s why we encourage you to watch for early signs of cataracts and see your eye doctor regularly. If you are experiencing vision changes or haven’t seen your eye care provider in the past year, schedule an appointment at your closest ECVA clinic today.