Cataract surgery has come a long way from its humble beginnings, evolving into a sophisticated procedure that combines medical expertise with cutting-edge technology. Cataract surgery in Western New York (WNY) has experienced significant advancements thanks to the evolution of digital technologies. Today, cataract surgeons in Buffalo, Orchard Park, Williamsville, and Niagara Falls have significantly transformed the landscape of eye care, particularly in cataract surgery.
This article explores the intersection of technology and eye care, delving into the innovations that are revolutionizing laser cataract surgery in the region.
Traditional Cataract Surgery in WNY: A Brief Recap
Cataracts occur when the eye lens becomes cloudy, leading to blurred vision and, in severe cases, blindness. The prevalence of cataracts tends to increase with age, making it a common condition among the elderly. Cataract surgery involves removing the cloudy lens and replacing it with an artificial intraocular lens (IOL) to restore clear vision.
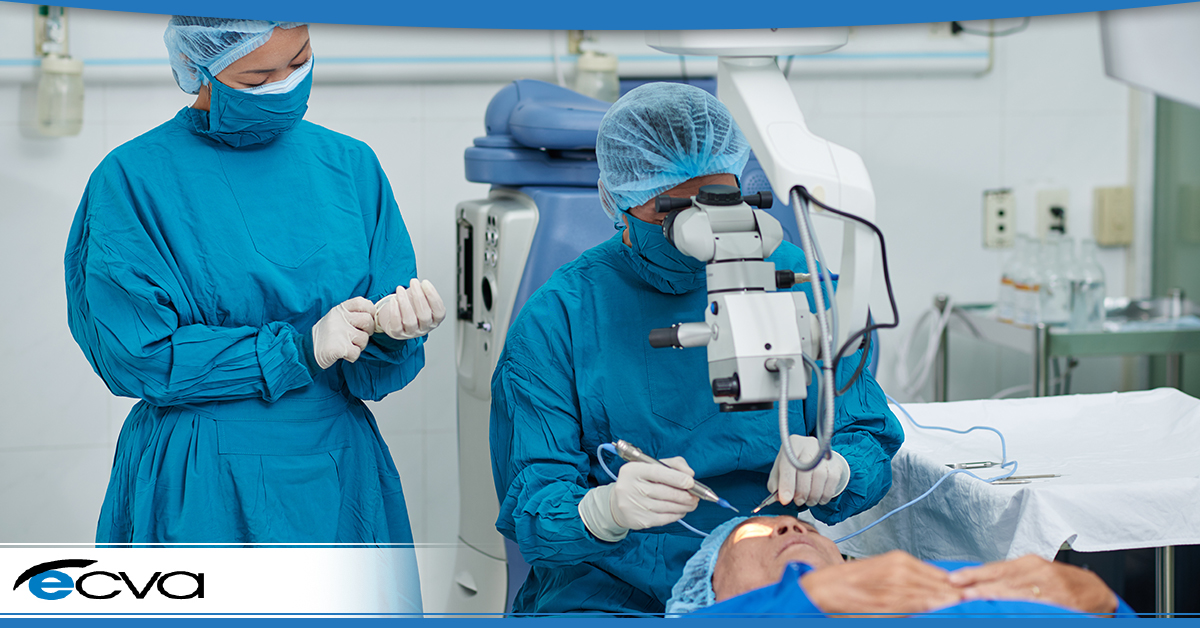
Traditionally, cataract surgery involves manual techniques performed by skilled surgeons using microsurgical instruments. While this approach has been successful for decades, integrating technology has enhanced precision, safety, and overall outcomes.
The Digital Transformation of Cataract Surgery in WNY
The landscape of cataract surgery in WNY is undergoing a profound transformation driven by the integration of today’s cutting-edge technologies. The digital revolution is reshaping how surgeons approach cataract procedures, emphasizing precision, safety, and personalized patient care. Some vital technological advancements are driving this transformation, from laser-assisted cataract surgery to artificial intelligence (AI) applications, advanced imaging technologies, enhanced intraocular lenses (IOLs), and the emerging role of 3D printing in customization. All of these tools stand to benefit patient outcomes, and while they are currently underutilized, that’s all about to change.
The Agency for Healthcare Research and Quality (AHRQ) says, “In the past several decades, technological advances have opened new possibilities for improving patient safety.” This evolution affects every area of medicine, including vision care.
As technology continues to evolve, the field of cataract surgery is embracing innovative solutions to enhance patient outcomes. Integrating advanced technologies aims to address challenges, improve surgical precision, and provide personalized treatment plans for individuals. This shift towards a technologically driven approach underscores the commitment to excellence in patient care, setting a new standard for cataract surgery in WNY.
Laser-Assisted Cataract Surgery
Laser-assisted cataract surgery (LACS) represents a groundbreaking development combining laser technology with traditional surgical techniques. Unlike traditional methods, LACS utilizes femtosecond lasers for critical steps in the surgery, including corneal incisions, capsulotomies, and lens fragmentation.
Before the surgery, detailed imaging of the eye is conducted using technologies like optical coherence tomography (OCT). This imaging provides a 3D eye map, allowing the surgeon to visualize the cataract and other structures more accurately.
The precision offered by lasers in creating incisions and performing delicate procedures has significantly enhanced surgical outcomes. Surgeons can now customize incision patterns, ensuring optimal wound healing and reducing astigmatism. Capsulotomies, the process of creating an opening in the lens capsule, are executed with unparalleled accuracy, contributing to improved IOL positioning and stability.
The femtosecond laser creates corneal incisions, the entry points for surgical instruments. These incisions are more precise than those made manually, promoting quicker healing and potentially reducing astigmatism. The laser is employed to make a circular opening in the front portion of the lens capsule, creating an access point for cataract’s removal. The precision of the laser in this step contributes to better centration of the intraocular lens. The femtosecond laser also fragments the cataractous lens into smaller, easily removable pieces. This can reduce the amount of ultrasound energy required during the surgery, potentially minimizing the risk of complications.
Incorporating robotics into cataract surgery further amplifies precision and safety. Robotic systems allow surgeons to control specialized instruments with utmost accuracy, navigating the complexities of the eye with finesse. The research states, “Robotic assistance can help overcome biologic limitations and improve our surgical performance.” Robotics technology minimizes the risk of complications and ensures the surgical reproducibility of results, setting a standard for excellence in surgical outcomes. The Ophthalmologist says, “By embracing developments such as robotics, healthcare providers can improve the quality of eyecare, empower surgeons, and raise surgical efficiency and reach.”
Examples of laser systems currently in use include the LenSx Laser System and the Catalys Precision Laser System. These systems have gained widespread acceptance for their efficacy in optimizing surgical steps and enhancing patient experiences.
Artificial Intelligence in Cataract Surgery
Artificial intelligence plays a pivotal role in the digital transformation of cataract surgery. In the preoperative phase, AI algorithms analyze patient data, including medical history and imaging results, to assist surgeons in formulating personalized treatment plans. This data-driven approach ensures that surgical strategies are tailored to individual patient needs, optimizing the chances of success.
AI contributes to intraoperative decision-making during laser cataract surgery by providing real-time insights and guidance. The integration of AI technologies allows for dynamic adjustments based on the evolving conditions of the eye, ensuring adaptability and precision throughout the procedure.
AI’s ability to process vast amounts of patient data enables the creation of personalized treatment plans. By considering factors such as ocular anatomy, refractive errors, and individual preferences, AI algorithms assist surgeons in selecting the most suitable IOL power and type. An AI-driven personalized approach enhances postoperative visual outcomes, minimizing the need for additional corrective measures.
When conducting cataract surgery in WNY, surgeons benefit from AI applications that assist in various aspects of cataract procedures. Computer-assisted guidance systems powered by AI help accurately place IOLs, ensuring optimal visual results. Additionally, AI-driven image recognition tools aid in identifying and differentiating subtle anatomical structures, contributing to enhanced surgical precision.
Advanced Imaging Technologies
The integration of advanced imaging technologies has revolutionized cataract surgery’s diagnostic and planning phases. Optical coherence tomography (OCT), in particular, has emerged as a valuable tool for visualizing the eye’s internal structures with high resolution.
OCT allows surgeons to visualize the anterior segment of the eye, including the cornea, iris, and lens, in three dimensions. This detailed imaging assists in precise surgical planning, guiding surgeons in determining optimal incision sites, IOL positioning, and overall strategy. The real-time feedback advanced imaging technologies provide enhances decision-making during surgery, improving outcomes and patient satisfaction.
Enhanced Intraocular Lenses (IOLs)
Intraocular lenses have evolved significantly, offering patients a range of options to address specific visual needs. Technological advancements have paved the way for premium IOLs that go beyond basic vision correction. These lenses are designed to address issues such as presbyopia and astigmatism, providing patients with a more comprehensive solution for their visual challenges.
Premium IOLs offer multifocality, enabling patients to see clearly at varying distances without additional corrective lenses. Additionally, IOLs with astigmatism correction capabilities further enhance visual acuity, ensuring a high quality of vision post-surgery. The availability of premium IOLs reflects a commitment to delivering functional vision and improved overall visual experience for patients in WNY.
3D Printing and Customization in Cataract Surgery
3D printing in cataract surgery is an exciting frontier that holds promise for customization and precision. This technology allows patient-specific models, enabling surgeons to visualize the unique anatomical features of each patient’s eye before the actual procedure.
Customization through 3D printing enhances surgical precision by providing surgeons with a tangible, three-dimensional representation of the patient’s eye. It allows meticulous preoperative planning, optimizing incision sites, IOL positioning, and overall surgical strategy. The ability to tailor surgical approaches to the specific characteristics of each patient’s eye contributes to improved outcomes and a more personalized surgical experience.
Pioneering cases and ongoing research in WNY showcase the benefits of 3D printing in cataract surgery. Surgeons are utilizing 3D-printed models to simulate and refine surgical techniques, ensuring a higher level of preparedness and confidence before entering the operating room. The ability to practice and tailor surgical approaches in a controlled environment contributes to the continued evolution of cataract surgery in the digital age.
Connect with a Leading Cataract Surgeon in WNY to Find Out if the Latest Advancements in Cataract Surgery are Right for You
The digital transformation of cataract surgery in WNY signifies a paradigm shift towards precision, personalization, and enhanced patient outcomes. From laser-assisted surgery and artificial intelligence applications to advanced imaging technologies, premium IOLs, and the emerging role of 3D printing, these technological advancements are collectively shaping a new era in laser cataract surgery.
Cataract surgeons in Buffalo, Orchard Park, Williamsville, Niagara Falls, and around the United States embracing these innovations will continue to reflect a commitment to excellence within the medical community. As cataract surgery in WNY continues to be at the forefront of the digital revolution in cataract surgery, integrating these technologies will likely become the standard of practice, setting a benchmark for eye care excellence nationwide.
Eye Care and Vision Associates offers our patients the best board-certified medical providers in the region. Our professional commitment to these cutting-edge technologies underscores their dedication to providing patients with the highest standard of care. Connect with the highly skilled cataract surgeons at ECVA with 4 conveniently located offices in Buffalo, Niagara Falls, Orchard Park and Williamsville today.